Sprains & Fractures
There are endless books regarding foot and ankle sprains and fractures. I will try to keep this brief and explore the more common injuries of the foot and ankle. I will spend extra time dedicated to lateral ankle sprains as this is the most common ankle injury I see.
First of all, what is the difference between a sprain and fracture?
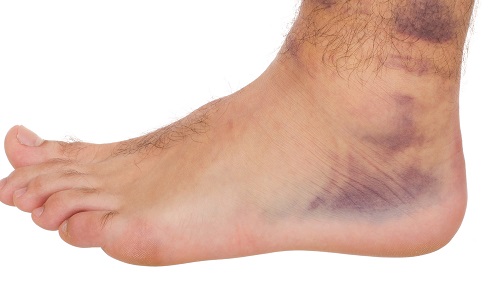
A sprain is a stretching of a ligament. A ligament is the tissue that connects bone to bone. Sprains are very common and can occur wherever there is a connection between two bones. Certain sprains are much more prevalent than others (ex: Lateral ankle sprains). A mild sprain stretches the ligament but leaves the joint stable. A moderate sprain is a partially torn ligament that can, in some instances, destabilize a joint. In a severe sprain, ligaments could tear almost completely, which may require surgery to repair.
Call Today to Schedule an Appointment
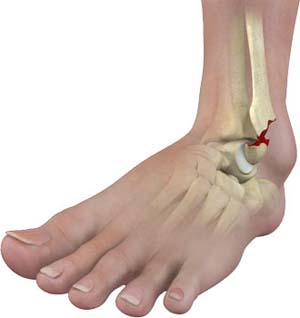
702 - 518 - 1862A fracture is simply a break in the bone. There are different types of fractures (displaced, non-displaced, oblique, spiral, comminuted, etc). Believe it or not, most fractures do not require surgery. Of course this depends on the severity and type of fracture, but most the time I see a fracture the patient will usually heal just fine with conservative treatment.
The most common fractures I see in the foot are metatarsal and phalanx (toe) fractures. Every now and then I will see fractures to the midfoot and rearfoot, and things can get quite tricky here as these tend to be more problematic. There is a fine art to diagnosing and treating fractures, as certain fractures are notorious for not healing and if improperly treated can lead to a lifetime of pain and complications. One of these notorious fractures is the Jones fractures, which is a fracture of the base of the 5th metatarsal. However, diagnosing this needs to be left up to a professional as the treatment of 5th metatarsal fractures is different based on location. The Jones fracture occurs at the metaphyseal – diaphyseal junction, an area that is notorious for having poor healing qualities due to the decreased blood flow. This often requires non-weightbearing in an offloading boot and close follow up as there is a higher than usual non-union rate (meaning the fracture doesn’t heal often requiring a bone stimulator or surgery). A fracture at the very base/tuberosity is an avulsion fracture and a 5th met shaft fracture is called a dancer’s fracture, both which heal easier than the Jones but still require proper treatment and could need surgery if severe enough.
Midfoot sprains and fractures can be nasty. One of the most often missed is the Lisfranc fracture. It is estimated this is missed 20-30% of the time! The Lisfranc ligament extends from the medial side of the base of the second metatarsal obliquely into the medial cuneiform. It is commonly believed to demonstrate either as a dorsal and plantar ligament or an interosseous ligament. It tends to be one or the other (most commonly interosseous). You can injury this area directly or indirectly. Indirect is more common which includes: Axial loading or twisting on a PF foot with forefoot abduction. Most common in MVA and sports injuries, as well as falling from a height. It is also common in equestrian times (foot caught in stirrup). An example of a direct injury is a crush injury (i.e. dropping something on the foot). Again, this injury is one of the more notorious injuries for causing problems and difficulty healing.


I’d like to discuss ankle injuries next. The most common ankle fracture I see is an isolated malleolar fracture, making up 2/3 of ankle fractures (bimalleolar making up 25%, and trimalleolar making up 7%). Most common cause is trauma with a supination, external rotation injury (SER). Again, several factors go in to determining the care of the fracture. If significantly displaced or the ankle is unstable, surgery is often needed. More often than not these isolated malleolar fractures do not require surgery, but an x-ray and full examination is absolutely essential in determining if surgical vs conservative treatment is needed.
I’d like to spend extra time on this last section discussing ankle sprains. The most common ankle injury I see (by far) is the lateral (inversion) ankle sprain. The lateral ankle sprain is the most ubiquitous injury in all of sport. Greater than 80% of all ankle injuries involve the lateral ankle with resulting stretching or rupture of the lateral ligamentous complex. At least 65% of chronic lateral ankle pain and instability is secondary to a previous ankle sprain, especially those that failed to undergo complete rehabilitation. Consequently, the number one risk factor for a lateral ankle sprain is a history of a previous sprain. Following the acute phase of an inversion ankle injury, aggressive rehabilitation featuring peroneal muscular strengthening and proprioceptive exercise is essential. It is easy for a person with an ankle injury to neglect physical therapy particularly when there is no pain, and this is often a mistake. I am a perfect example of this as I injured my ankle in high school in a basketball game but didn’t do physical therapy as I had no pain and I never saw a doctor for the injury. What a mistake it was as I kept re-twisting my ankle and never understood why (and I was wearing ankle braces!). Finally, I saw a podiatrist (before I was a podiatrist obviously) and I did physical therapy and I’m yet to re-sprain it (knock on wood!).
When conservative treatment fails, delayed primary surgical repair of the lateral ligaments is indicated. Although ligamentous sprain and/or rupture is most common with the inversion mechanism of injury, several other associated injuries are frequently encountered. These include avulsion fracture of the fifth metatarsal base, Jones fracture, syndesmosis injury, calcaneal anterior process facture, talar lateral process fracture, talar dome fracture, peroneal or flexor tendon injury and sural nerve damage. Other mechanisms of ankle sprains are uncommon and include the medial (eversion) ankle sprain and anterior or posterior ankle impingement injury
Prior to examination, scout radiographs should be taken to exclude the possibility of ankle fracture/dislocation or subtalar dislocation. Anterior-posterior, medial-oblique and lateral views of the ankle along with a medial-oblique view of the foot should be obtained. Thorough examination of a lateral ankle injury should begin proximally and at the suspected least painful areas. Palpation of the proximal fibula is necessary to exclude a Maisonneuve fracture, most commonly seen with pronation – external rotation of the ankle. The medial ankle should then be explored with careful assessment of the deltoid ligament, spring ligament and tibialis posterior tendon. The anterior talofibular,
calcaneofibular and posterior talofibular ligaments and tibiofibular syndesmosis should then be palpated. If injury to the syndesmosis is suspected, the squeeze test, tibiotalar shuck test, external rotation test or fibular mobilization may be performed to confirm this possibility. The presence of ankle diastasis radiographically is highly suggestive of rupture. The anterior drawer test or “push-pull” test should then be performed with careful attention to “dimpling” of the skin overlying the lateral malleolus. Although this should be compared to the uninjured ankle, the comparison is of questionable significance if there is also a history of previous ankle inversion injury. Upon completing the ankle evaluation, the injury may then be clinically graded: Grade I injury is defined as a mild strain or stretching of the anterior talofibular ligament only. A grade II lateral ankle injury consists of a complete tear of the anterior talofibular ligament and a stretch injury to the calcaneofibular ligament. A grade III injury is defined as complete rupture of the anterior talofibular and calcaneofibular ligaments, with a resulting unstable ankle. Some authors have described a type IV injury that includes partial/complete rupture to the posterior talofibular ligament resulting in an unstable ankle. By grading the ankle sprain, a clearer prognosis may be established for full recovery and return to athletic participation.
Often with more serious sprains an MRI is ordered. If I suspect more of a bone/fracture injury then a CT scan is often ordered. Stress radiography may be helpful to confirm anatomical instability. The patient must be anaesthetized (common peroneal block) and have a negative history of injury to the contralateral ankle. The anterior drawer (push-pull) examination is specific for the anterior talofibular ligament only. 4 mm or more of anterior displacement of the talus (when compared to the contralateral side) is considered positive (abnormal). The inversion stress examines primarily the calcaneofibular and posterior talo-fibular ligaments. An inversion stress (talar tilt) of 10 degrees is positive for calcaneofibular sprain and a talar tilt of 15 degrees or greater indicates complete calcaneofibular disruption (grade III) sprain. For example, a grade I injury would have a (+) PP and a (-) inversion stress. Chronic lateral ankle instability may be categorized as either functional or mechanical (structural). The stress examination only evaluates the potential for mechanical instability. Functional instability may occur do to damage to the proprioceptive nerve endings located in the skin overlying the lateral ankle ligaments (and on the sole of the foot, interestingly enough). Rehabilitation allows for re-education and healing of these structures. Studies have indicated that pain contributes to ankle instability and that anesthetic blockade of the ligaments and sinus tarsi provides increased ankle stability in these cases
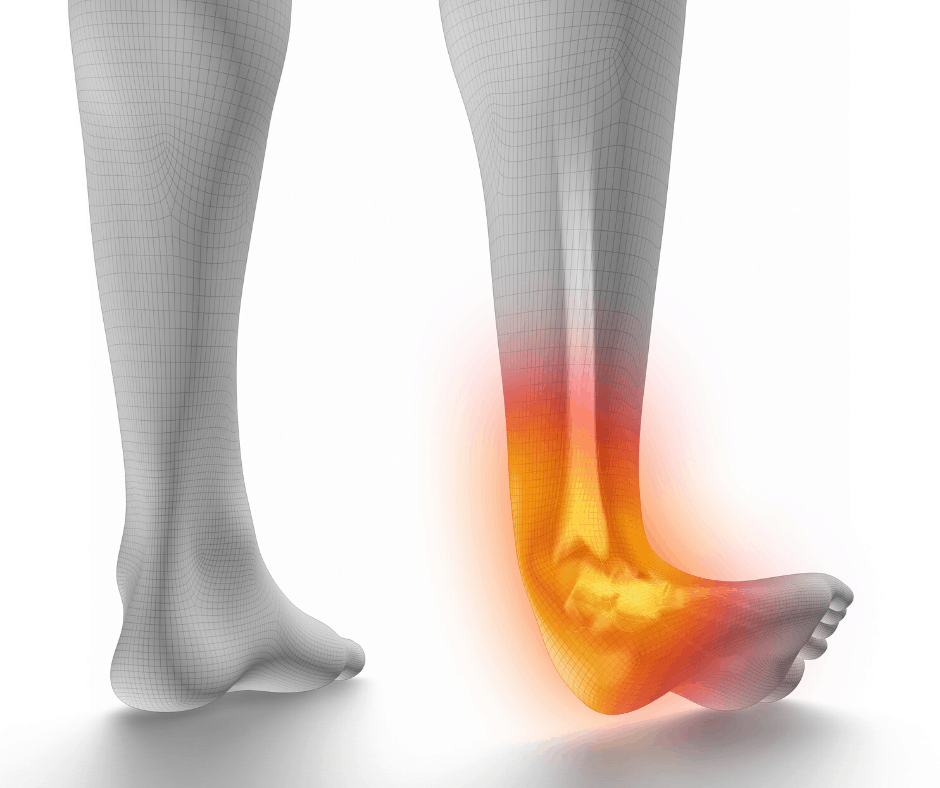
The acute ankle injury should be managed initially following the PRICE principle: Protection, Rest, ice, compression and elevation. Non-steroidal anti-inflammatory medication may also be used to reduce edema and pain. If the patient is unable to bear weight, a compression dressing should be applied for up to seven days. The period of non-weight bearing should be limited as much as possible. A CAM walker should be applied and weight bearing encouraged as soon as possible. This is important for two main reasons: The CAM walker or “boot” allows for early weight – bearing and provides protection. Also, it maintains the ankle in a dorsiflexed position and therefore keeps the anterior talo-fibular ligament well approximated. If the ankle is in a plantarflexed position, the patient will have more pain and potentially heal at a slower rate. If injury to the syndesmosis is suspected, cast immobilization for 4 – 6 weeks is recommended. Associated injuries, such as talar dome or fifth metatarsal styloid fractures should be addressed at this time. Due to the ligamentous damage, chronic lateral ankle pain and instability is perhaps the greatest potential complication of inversion ankle sprains. An inversion ankle sprain results in some degree of functional and anatomic instability. This underscores the need for aggressive rehabilitation and physical therapy which follows distinct phases. Phase I of rehabilitation is aimed at reducing pain and edema and employs elements such as contrast bathing, interferential stimulation, range of motion exercise and pneumatic compression . Phase II consists of strengthening and stretching exercises, massage and basic proprioceptive exercise. Phase III involves more advanced strengthening and proprioceptive exercise, trampoline, jumping rope and BAPS (biomechanical ankle platform system) board. Peroneal muscular strengthening and proprioceptive exercise are the most essential elements of ankle sprain rehabilitation and prevention. Phase IV involves sport-specific exercise and preventative strategies such as braces, taping, high-top shoes and functional foot orthoses. In most cases, the ankle should be “protected” for up to six months following an injury. Braces are clearly more effective than tape, orthosis and high-top shoes in preventing lateral ankle injury. Although they provide some direct support, braces and tape primarily increase peroneal reactivity. Patients generally require somewhere between 4 –8 weeks of rehabilitation (3 times/week). In some cases (grade III) additional therapy may be necessary.
Several anatomical and biomechanical factors play a role in the tendency toward ankle inversion injury. The ankle joint consists of the talar dome articulating with the tibial plafond. The ankle joint axis is angled almost 90 degrees from the sagittal plane, resulting in primarily dorsiflexion and plantarflexion. Minimal frontal plane (inversion, eversion) motion is available at the ankle joint. Inversion and eversion occur at the subtalar joint, which provides a varus or valgus force upon the ankle. Normally, the amount of subtalar inversion exceeds that of eversion by a ratio of 2:1. This increases the likelihood of an inversion-type injury to the ankle and subtalar joints. Forefoot valgus, rearfoot varus and ankle equinus may also contribute to lateral ankle instability due to the supinatory force placed on the subtalar joint. The talar dome is wide anteriorly and narrow posteriorly when viewed from above. When the ankle joint is dorsiflexed, the wider anterior aspect of the talus fits firmly in the ankle mortise. When the ankle is plantarflexed, the talar dome is less stable in the ankle mortise and consequently an inversion ankle injury most commonly occurs when the ankle is in plantarflexion (inversion-plantarflexion). Anatomically, the lateral ankle consists of three ligaments, the anterior talofibular, calcaneofibular and posterior talofibular ligaments. These structures provide stability to the lateral ankle and subtalar joint. The peroneal muscles provide additional stability to the lateral ankle and appropriate peroneal muscular reactivity is essential in preventing inversion ankle injury. Injury to the anterior – inferior tibiofibular syndesmosis is referred to as a “high” ankle sprain and is not uncommon when the ankle is subjected to a severe inversion force. The medial ankle is fortified by the deltoid ligament which consist of five separate ligaments. Medial (eversion) ankle injuries rarely result in significant ligamentous compromise nor require any long-term treatment. The tibialis posterior tendon is much more likely to be injured and should be thoroughly evaluated following
any eversion sprain. Anterior ankle impingement may occur with forced ankle dorsiflexion but is more commonly a chronic, overuse type of injury. Posterior impingement may likewise occur with repeated ankle joint plantarflexion, such as seen in releve. Injury to the flexor hallucis longus tendon and the presence of a retrocalcaneal bursitis or os trigonum must be excluded in the diagnosis when posterior ankle pain is present.
When can the patient return to activity? This is the “million-dollar question” because it has not been clearly defined. This is especially important question with athletes as the amount of stress and strain at the area requires a fully rehabbed ankle with specific tests that need to be performed before they can start back their sport. I base my decision on a few factors. One of these factors is patient must be able to walk quickly without pain or a limp. Second, the patient must be able to perform a single – leg toe raise and with athletes to be able to balance on his/her forefoot while jumping up and down. There are several other factors, clinical findings, and tests I have and a patient’s lifestyle (athlete vs sedentary patient) will weigh heavily into my decision.
When conservative care fails resulting in chronic lateral ankle pain and/or instability delayed surgical repair of the lateral ligaments is indicated. Rarely (never say never, but almost never!) is immediate repair of the lateral ankle ligaments appropriate, as rehabilitation yields excellent/acceptable results in the vast majority of cases. Studies have shown that repairing the anterior talofibular ligament is most essential, whereas repairing the calcaneofibular ligament does not provide any additional benefits. Several surgical techniques, including the modified Brostrom procedure, involve repair of the anterior talofibular ligament and reinforcement of the lateral ankle with a portion of the extensor retinaculum. Alternative surgical methods, referred to as stabilization techniques, involve reinforcing the lateral ankle with a portion or the peroneus longus or brevis tendon. However, these techniques are more technically difficult, compromise the integrity of the normal anatomy and increase the risk of over-tightening the ankle. The current literature clearly favors the Brostrom-type procedures which produce excellent outcomes without the associated technical difficulty or potential postoperative complications.
As a 24/7 house & hotel Las Vegas Podiatrist I take pride in my thorough evaluation and treatment of toe pain and ingrown toenails. My treatment of ingrown toenails are backed by peer reviewed journals and research and in my opinion are the best treatment of ingrown toenails. I do not use “cheap” supplies and my inventory is stocked with only the most up to date and high quality supplies.
Please call now if you are around Las Vegas and suffer from heel pain, plantar fasciitis, neuroma, ingrown toenail , painful nails , warts, thick and long fungal nails, diabetic feet , or an ankle sprain. For information on what/why I use for my chemical matrixectomies for ingrown nails please visit this link.
SCHEDULE YOUR CONSULTATION
